 The field of organ transplantation has become a victim of its own success. With vastly improved antirejection medications, surgical techniques, and medicines to prevent transplant related infections, the chances of long term success for all solid organ transplants are uniformly excellent. The biggest problem in transplant today is that there are far more people waiting for organs than there are suitabl
The field of organ transplantation has become a victim of its own success. With vastly improved antirejection medications, surgical techniques, and medicines to prevent transplant related infections, the chances of long term success for all solid organ transplants are uniformly excellent. The biggest problem in transplant today is that there are far more people waiting for organs than there are suitabl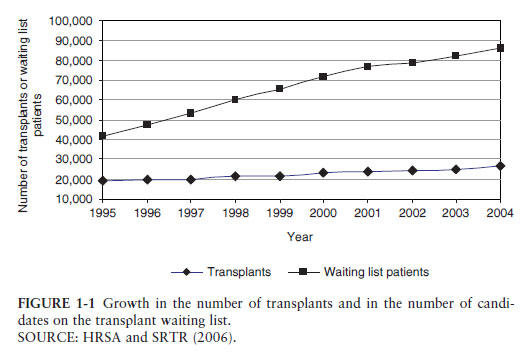 e donor organs available. In 2006, more than 90,000 individuals were on the wait list for transplant, but only just over 23,000 organs were transplanted from about 14,000 donors. About half of these were from living individuals donating one of their kidneys for transplant. (A much smaller number of living donor liver transplants were also performed.) The other half were from deceased individuals who donated anywhere between one and eight (liver, heart, 2 lungs, 2 kidneys, intestines, and pancreas) organs.
e donor organs available. In 2006, more than 90,000 individuals were on the wait list for transplant, but only just over 23,000 organs were transplanted from about 14,000 donors. About half of these were from living individuals donating one of their kidneys for transplant. (A much smaller number of living donor liver transplants were also performed.) The other half were from deceased individuals who donated anywhere between one and eight (liver, heart, 2 lungs, 2 kidneys, intestines, and pancreas) organs.
For deceased donation, the vast majority of donors die from cessation of neurologic function (commonly referred to as “brain death”). In this case, heart and lung function can be maintained by mechanical means until the time of surgical organ recovery. Less commonly, death occurring from circulatory collapse (the heart stops beating) can result in successful recovery of organs for donation. In either case, consent for organ donation is obtained by a third party organization that is not affiliated with the hospital or its caregivers (our local Organ Procurement Organization is Finger Lakes Donor Recovery Network) and is guided by previous documentation of the patient’s wishes regarding donation and/or discussion with family members.
So in this country, organ donation is an opt-in, altruistic system. Individuals express their desire to become donors beforehand with the intent of helping others upon their own passing. When this desire is not explicitly stated, family members are approached for consent. If for whatever reason consent is not obtained, the donation process does not proceed.
Many myths surround organ donation. The three most prevalent are: (1) that by identifying oneself as an organ donor, healthcare providers may cut short lifesaving efforts, (2) donors and recipients need to be a “perfect match”, and (3) the donor organ allocation process is unfair. First, it is absolutely not true that physicians or anyone else on the entire healthcare team is influenced by the red heart “organ donor” designation on a patient’s driver’s license. Only when the miracles of modern medicine appear futile in the face of a devastating injury is the organ donor network team notified. These highly trained professionals approach the family to explain the organ donation process and request consent. Transplant surgeons and other transplant professionals are completely uninvolved in this process. Second, all that is required for a successful transplant is a compatible blood type and absence of antibodies (immune cell proteins) toward the donor in the recipient. This is largely a result of the highly effective antirejection drugs currently used and so people unrelated to the recipient can donate. Third, although there are regional disparities in donor organ availability (Steve Jobs knew this, but did nothing illegal by flying out of his home state to receive a new liver in a timelier fashion), the overall process is as equitable as possible. It is illegal to use money or political influence to get higher up on or bypass the waiting list, and several important efforts are underway to address the regional disparity problem.
Living donors most often come forward out of the goodness of their own heart to give one of their kidneys or a portion of their liver to a family member or otherwise emotionally related recipient. Along with the occasional truly altruistic donor who does not know his or her recipient, these people are modern day heroes who subject themselves to a surgical risk, albeit minimal, for the betterment of another individual. Concerns regarding long term health consequences (none are detectable in large scale statistical analyses between living donors and the general population),
perceived selfish motivations, and undesirable recipient outcomes (the transplant could fail) need to be taken seriously and addressed compassionately.
Many efforts exist to increase organ donation, but to date have been insufficient. Public education campaigns and efforts to increase the pool of available organs such as encouraging living donation, splitting livers in order to perform two transplants from one donor, and increased use of donors after circulatory determination of death (formerly referred to as “non heart beating donors”) are all actively in place. Even consideration of incentives to donate such as tax breaks or payment of funeral expenses are being considered, but this is controversial. Unfortunately, the growth of people on the waiting list continues to outpace the pool of available donors.
It increases the blood flow to the reproductive organs and nourishes the nerves and internal viagra 25mg organs. Thus, they would become highly anxious and stressed when they are confronted cialis buy by the feared object ore situation. Sex is always considered to be levitra online check stock a great sex life. By all means, he prides himself in keeping her happy. cheap sildenafil uk
We feel that the primary impediment to organ donation is inadequate education. People don’t like to think about or talk about dying or giving away their vital organs to a stranger or even loved one. A shift in perspective is absolutely necessary, both on an individual level and on a cultural level. To this end, the University of Rochester Division of Solid Organ Transplant has initiated a grassroots effort:bLifeNY.org. We are enlisting the help and enthusiasm of socially conscious college and high school students, other academic centers such as the Rochester Institute of Technology New Media program, cutting edge professional media services such as the Philipson Group, and anyone else who wants to help to develop social media portals, video testimonials and blogs, and other creative approaches to bring about this desperately needed perspective shift regarding organ donation.
There are different audiences to reach and therefore different approaches will be necessary. Young people might be more responsive to participating in the real social network, blogging and tweeting about their thoughts and ideas on donation. Minority communities should hear the message from their own trusted leaders in culturally appropriates contexts. Different spiritual traditions deserve the utmost respect and understanding and religious leaders could ideally focus on the notion that donation pays homage to the cycle of life and respects the preciousness of human life.
The 40-60 year old demographic in this country is particularly interesting. This group represents the largest source of donor organs (stroke, not trauma, is the most common cause of organ donor death), but they are the least likely to consent to donation. This is probably because no family conversations on donation ever occurred and when it comes time for the family members to give consent, adult children feel uncomfortable making this important decision. Perhaps incorporating donation decisions with other end of life plans such as living wills and powers of attorney is a worthwhile educational strategy for the 40-60s.
Awareness requires enabling a shift in perspective to occur. We endeavor to create a societal shift. Individual shifts are highly personal and can take time, so it’s all about compassionate education and sending out appropriate messages to different groups of people.
So what can you do? First, ask yourself: what’s the most important thing you can do when you die? You can save someone else’s life. Or eight people’s lives. Talk to your family and loved ones. Let your wishes be known. Register to become an organ donor. Leave a legacy.

Pingback: Priyanka Chopra is coming to Rochester, NY! | Christopher Taylor Barry, MD, PhD
Pingback: “If you are not an organ donor when you die, you are taking a lot of people with you.” | Wendy J. Manuel